
Physiotherapy (12)
TMJ, or temporomandibular joint disorder, is a common condition that can cause pain and discomfort in the jaw and face. Fortunately, physiotherapy can be an effective treatment for TMJ, and the process of getting help can be fun and upbeat. In this blog, we'll explore how physiotherapy benefits those with TMJ and how it can be a positive experience.

First, let's talk about what TMJ is. The temporomandibular joint connects the jawbone to the skull and allows you to open and close your mouth. When this joint isn't functioning properly, it can cause pain, stiffness, and difficulty chewing. TMJ can be caused by a variety of factors, including injury, stress, teeth grinding, or arthritis.
Physiotherapy is a form of treatment that involves exercises, manual therapy, and other techniques to help relieve pain and improve mobility.
When it comes to TMJ, physiotherapy can help by:
Reducing pain: A physiotherapist can use manual therapy techniques like massage and stretching to alleviate pain in the jaw and surrounding muscles.
Improving jaw mobility: Through targeted exercises and stretches, a physiotherapist can help increase the range of motion in the jaw, making it easier to open and close the mouth.
Addressing underlying causes: If TMJ is caused by an underlying issue like teeth grinding or poor posture, a physiotherapist can help address those issues and prevent future problems.
Physiotherapy can be a positive experience for those with TMJ, for a few reasons:
The exercises and techniques used in physiotherapy will help lossen your jaw muscles and improve jaw function.
Physiotherapy is a social experience. You'll be working with a physiotherapist who can guide you through exercises and offer encouragement and support.
If you're dealing with pain and discomfort from TMJ, it can be frustrating and discouraging. But by taking action and seeking treatment, you can regain a sense of control over your health and well-being.
In summary, TMJ can be a painful and frustrating condition, but physiotherapy can be an effective way to address it. With the help of a skilled physiotherapist, you can reduce pain, improve mobility, and feel better overall.
So don't hesitate to seek out physiotherapy if you're dealing with TMJ – it could be just the solution you need!
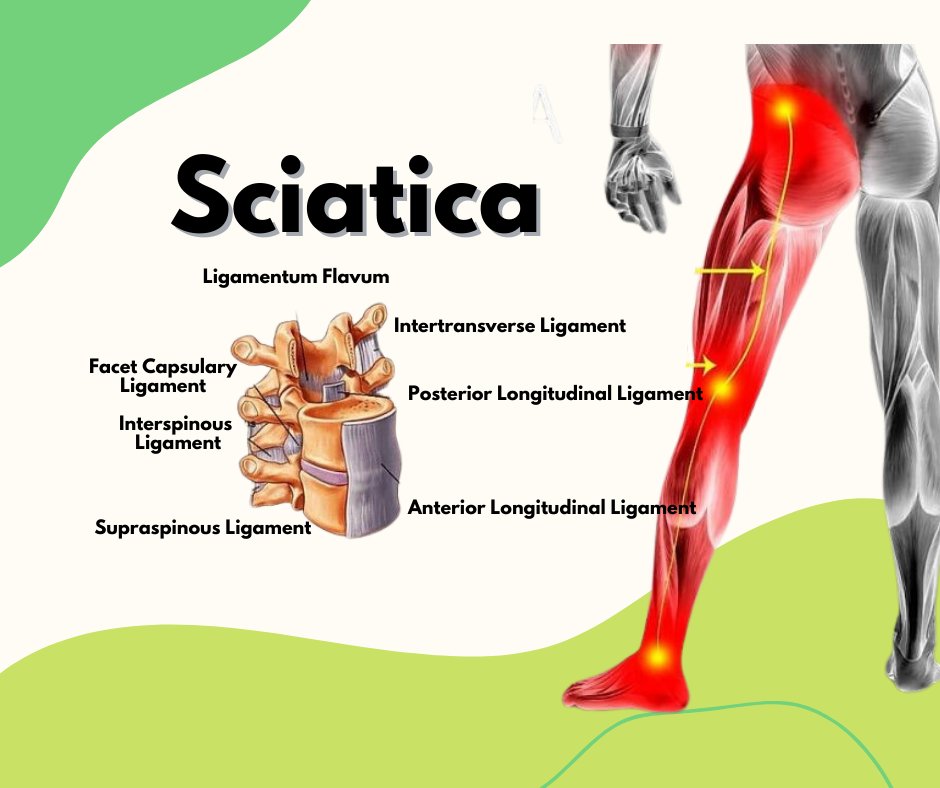
Are you feeling like you've got a rock in your shoe, even when you're not wearing any? Do you dread getting out of bed in the morning because of that sharp pain in your heel? If so, you might be one of the millions of people suffering from plantar fasciitis. Don't worry, though – it's a common condition that can be easily treated with the help of physiotherapy.
So what is plantar fasciitis, anyway? Simply put, it's an inflammation of the plantar fascia, which is the band of tissue that connects your heel bone to your toes. When that tissue gets inflamed, it can cause a lot of pain and discomfort, especially when you're on your feet for long periods of time.
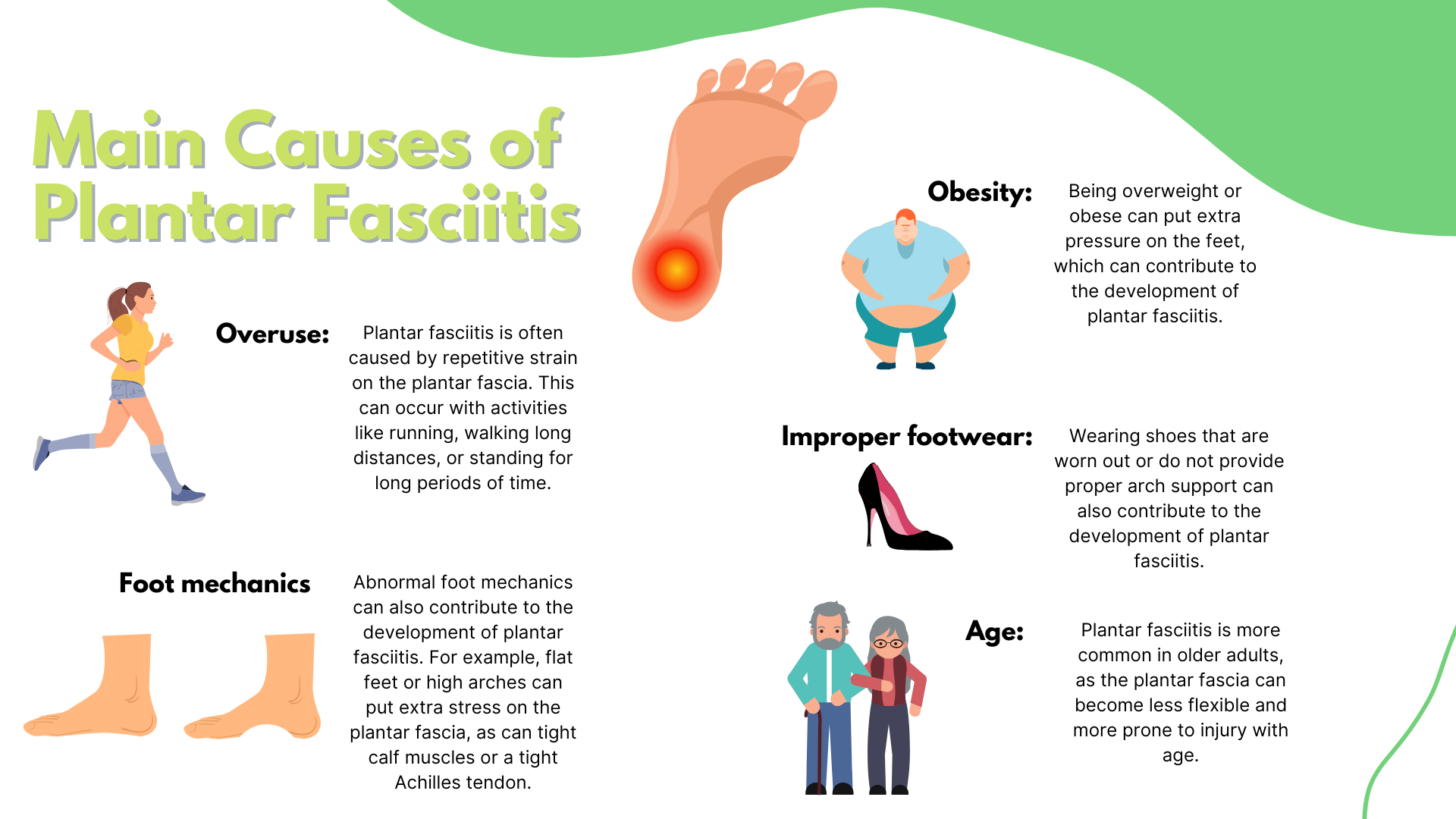
But fear not! There are plenty of ways to treat plantar fasciitis, and physiotherapy is one of the most effective methods. Here are just a few of the ways that physiotherapy can help:
Stretching exercises: One of the key causes of plantar fasciitis is tight calf muscles, which can put extra strain on the plantar fascia. A physiotherapist can help you stretch out those muscles, which can help to relieve some of the pressure on your heel.
Massage therapy: Massaging the affected area can also help to loosen up tight muscles and reduce inflammation. Your physiotherapist may use various techniques, such as deep tissue massage or trigger point therapy, to help ease your pain.
Custom orthotics: If you have flat feet or high arches, your physiotherapist may recommend custom orthotics to help support your feet and reduce the pressure on your heels.
Strength exercises: Building up the strength in your feet and calves can also help to alleviate plantar fasciitis. Your physiotherapist may recommend specific exercises, such as heel raises or toe curls, to help strengthen the muscles in your feet.
Shock wave therapy:In addition to the physiotherapy techniques we've already discussed, shock wave therapy is another treatment option that can be highly effective in treating plantar fasciitis.
So what is shock wave therapy, exactly? It's a non-invasive treatment that uses high-energy sound waves to stimulate the body's natural healing processes. When these sound waves are applied to the affected area, they can increase blood flow and reduce inflammation, which can help to promote healing.
In the case of plantar fasciitis, shock wave therapy has been shown to be particularly effective in relieving pain and improving function. In fact, a recent study found that patients who received shock wave therapy for their plantar fasciitis experienced significant reductions in pain and disability, compared to those who received a placebo treatment.
While the exact mechanism behind shock wave therapy's effectiveness for plantar fasciitis is not yet fully understood, it's thought that the treatment may help to break up scar tissue and stimulate the growth of new tissue in the affected area. This can help to relieve pain, reduce inflammation, and improve overall function.
If you're considering shock wave therapy for your plantar fasciitis, it's important to work with a qualified healthcare professional who can assess your specific needs and determine the best course of treatment for you. But for many patients, shock wave therapy can be a highly effective way to relieve pain and improve their quality of life.
Education and advice: Finally, your physiotherapist can provide you with education and advice on how to manage your symptoms and prevent further injury. They can show you proper techniques for stretching and strengthening your feet, as well as recommend footwear and lifestyle changes to help reduce your risk of developing plantar fasciitis again in the future.
So there you have it – plantar fasciitis may be a pain in the heel, but with the help of a physiotherapist, you can get back on your feet in no time. Don't suffer in silence – book an appointment today and start feeling better!
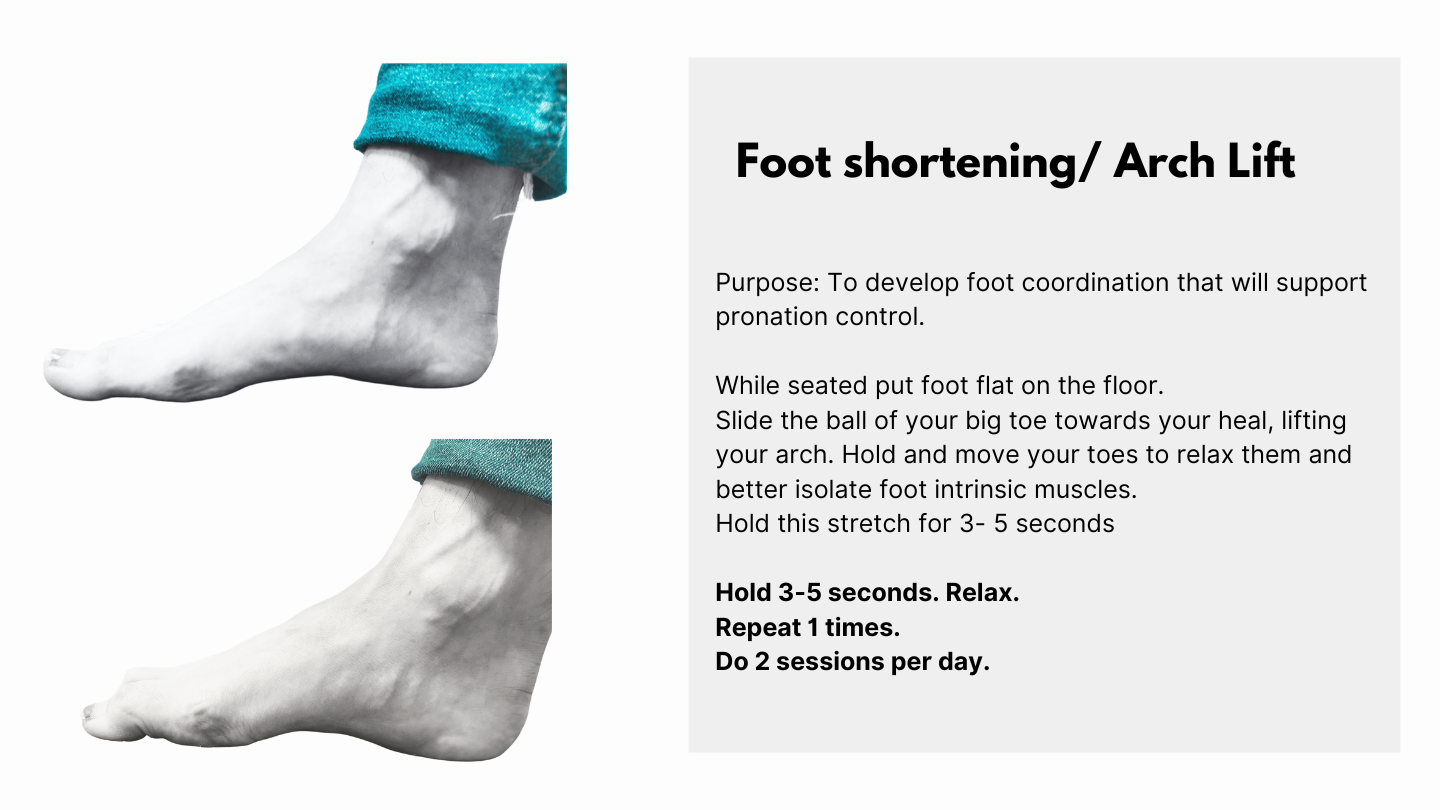
Exercises for Plantar Fasciitis
Please note that it's important to consult with a healthcare professional before starting any new exercise program, especially if you're experiencing pain or discomfort.




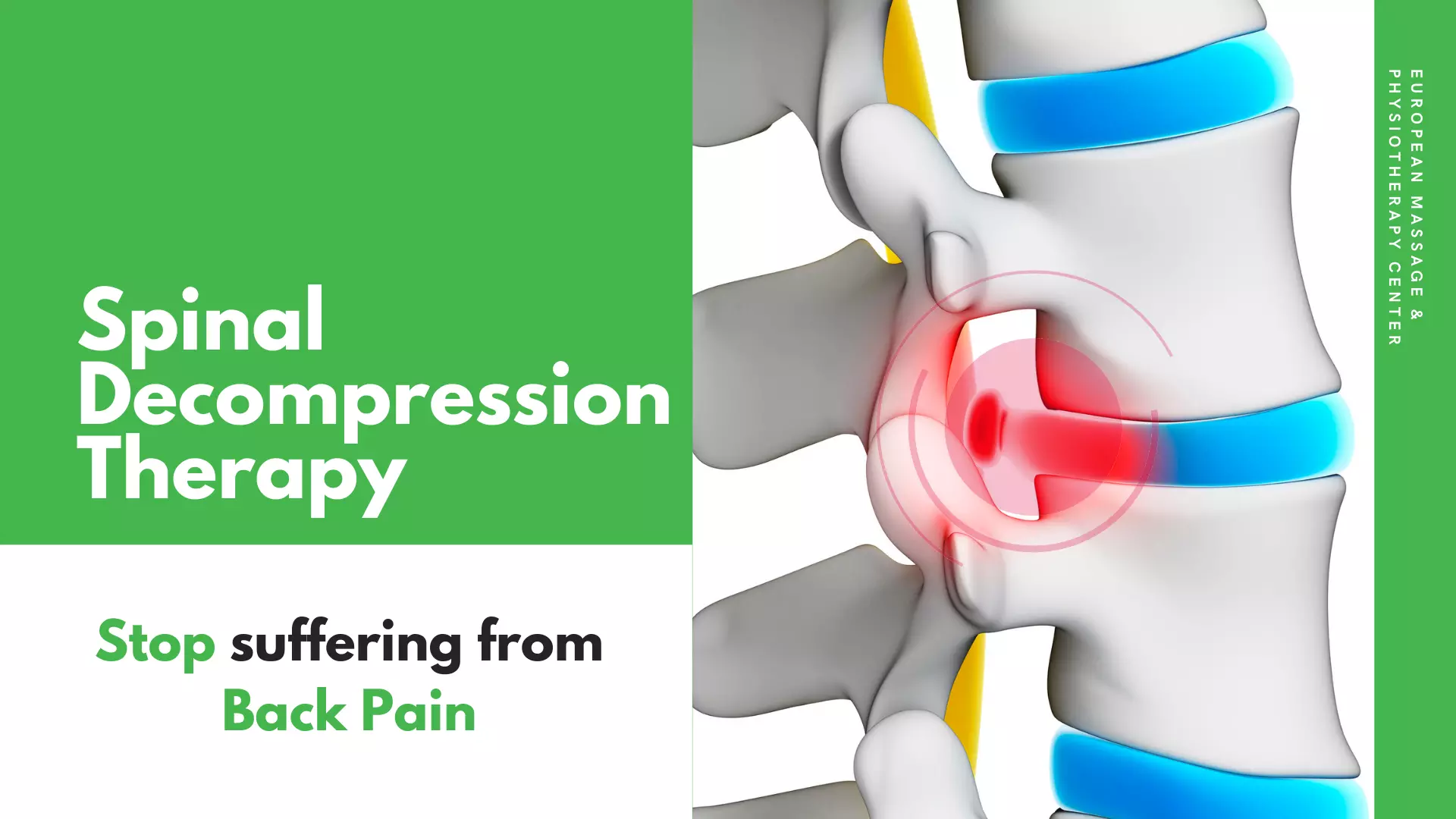
Spinal Decompression Table: A Solution for Back Pain
Back pain is a common problem affecting millions of people worldwide. While there are several ways to manage it, one of the most effective is through the use of a spinal decompression table. This therapy uses traction to stretch the spine, relieve pressure, and promote healing. In this blog, we will discuss what a spinal decompression table is, how it works, and its numerous benefits.

What is a Spinal Decompression Table?
A spinal decompression table is a specialized medical device designed to relieve back pain. It uses traction to stretch the spine and reduce pressure on the vertebrae and discs. The table is equipped with a motor that can be controlled to adjust the amount of traction applied to the spine. The patient lies down on the table and is secured with straps, which help to keep them in place during the therapy session.
How Does Spinal Decompression Work?
The spinal decompression table works by creating a negative pressure within the discs, which helps to pull the herniated or bulging discs back into their proper position. As the spine is stretched, the pressure on the discs is reduced, and the discs are able to rehydrate, which promotes healing. Over time, this can lead to a reduction in pain and an improvement in mobility.
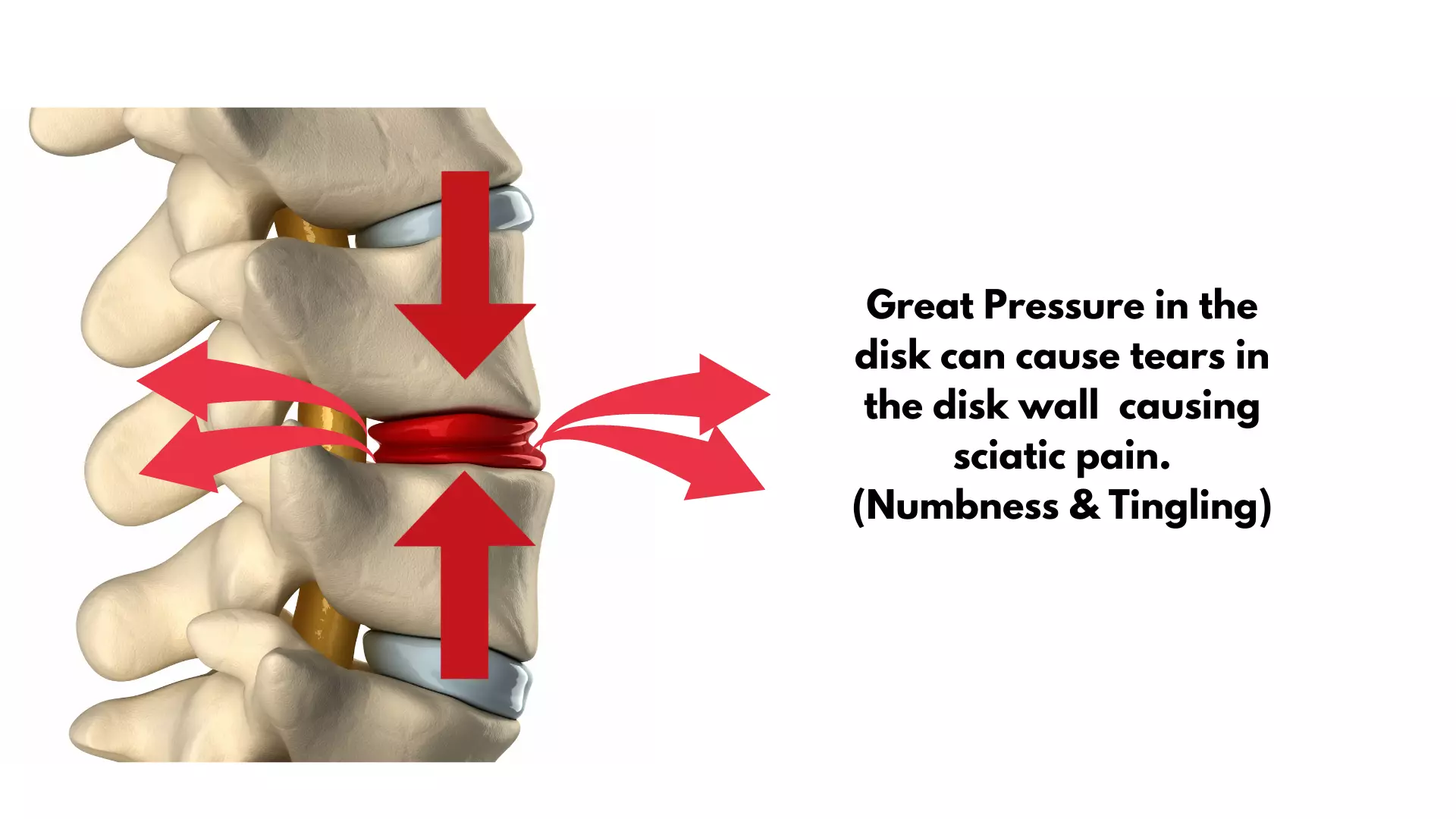
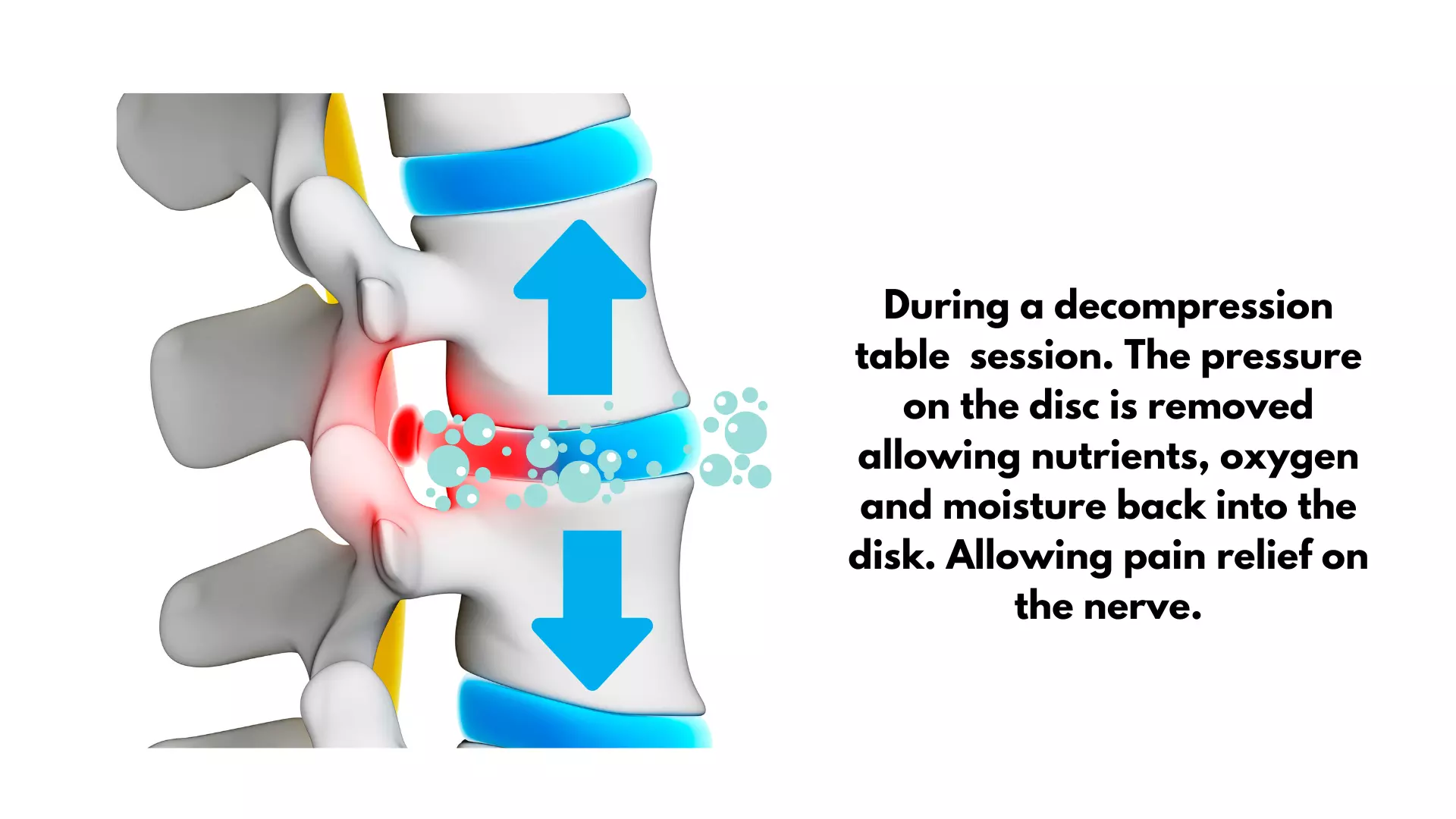
Benefits of Spinal Decompression Table
- Relief from Back Pain: Spinal decompression therapy has been shown to be effective in reducing back pain caused by herniated discs, bulging discs, sciatica, and other conditions.
- Non-Invasive: Unlike surgery, spinal decompression is non-invasive and does not require any incisions or anesthesia.
- Safe: Spinal decompression is considered a safe form of therapy with minimal side effects. It is also a low-risk alternative to surgery.
- Improved Mobility: As the pressure on the discs is reduced, patients can experience improved mobility, allowing them to move more freely and with less pain.
- Long-Term Results: Unlike medications that only provide temporary relief, spinal decompression can lead to long-term results, reducing the need for ongoing treatment.
In conclusion, a spinal decompression table is a safe and effective way to manage back pain. It offers numerous benefits, including relief from pain, improved mobility, and long-term results. If you are suffering from back pain, consider spinal decompression therapy as a potential solution.
Note: It is important to consult with a medical professional before starting any form of therapy to ensure that it is safe and appropriate for your specific condition. Call and book a free consultation with one of our physiotherapist!

Have you ever felt tingling, numbness, electrical currents, burning or a combination of all sensations in your fingers or hands?
Has the feeling persisted over months and is getting worse?
Carpal tunnel starts out slowly and gradually. You may feel numbness and weakness in your fingers and hands. Carpal tunnel is a painful condition that usually get worse overtime if left untreated. Untreated carpal tunnel can lead to permanent nerve damage.
Carpal tunnel syndrome is a disorder that affects the hand, wrist, and arm caused by pressure on the median nerve in the wrist. It can cause pain, numbness, and tingling in the fingers and thumb, as well as weakness in the hand. Early signs of carpal tunnel psyndrome can include pain, tingling, or “pins and needles” sensations in the palm, thumb, index and middle fingers, as well as aching, burning, and numbness in the wrist.Physiotherapy is an important part of treatment for carpal tunnel syndrome. Physiotherapists can assist in the diagnosis and management of carpal tunnel syndrome through patient education, activity modification, and exercise. Education is key to understanding carpal tunnel syndrome and avoiding activities that can worsen symptoms.


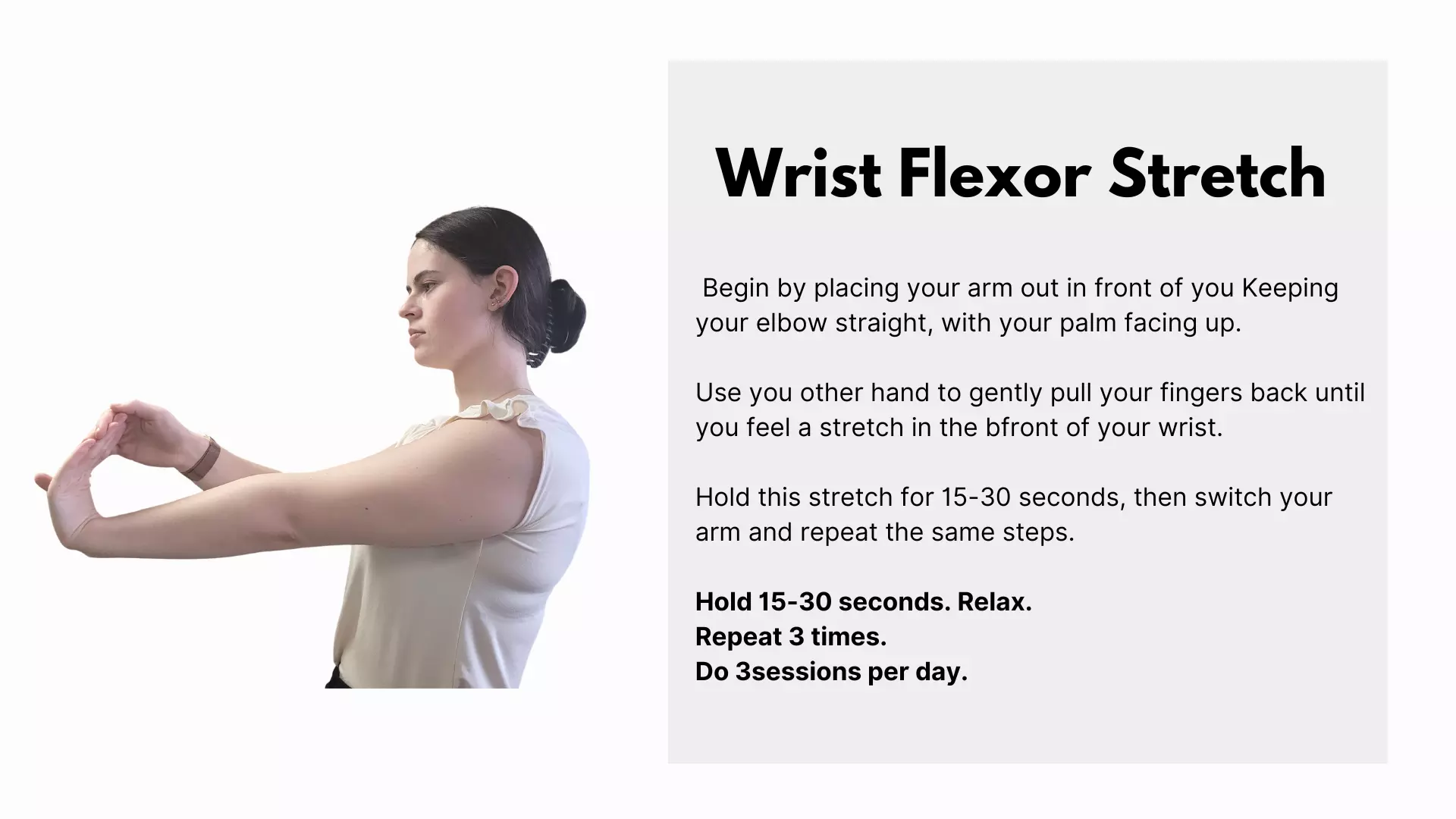

Try these exercises at home, or ask your physiotherapist to show you how to do them properly. Just remember slow and steady wins the race. Don't push yourself too hard, and listen to your body. If you were unable to do the modality due to increased pain stop immediately. If pain increases contact your physiotherapist or physician. If you have any questions call us for a free consultation with one of our Physiotherapists.
Are you constantly hunched over looking down on your phone or other devices and feeling the pains and strains in your neck?
What is Text neck?
Text neck pain is a real symptom. Our head is the heaviest part of the body and the muscles and ligaments are not designed to hold it for long periods of time in a position where you are looking down.
When you lean forward while using your cell phone for prolonged periods of time, this is a form of repetitive strain injury that causes neck and shoulder pain that can lead to tension headaches in some cases.
Text neck is a lifestyle problem that can be treated by a physiotherapist.
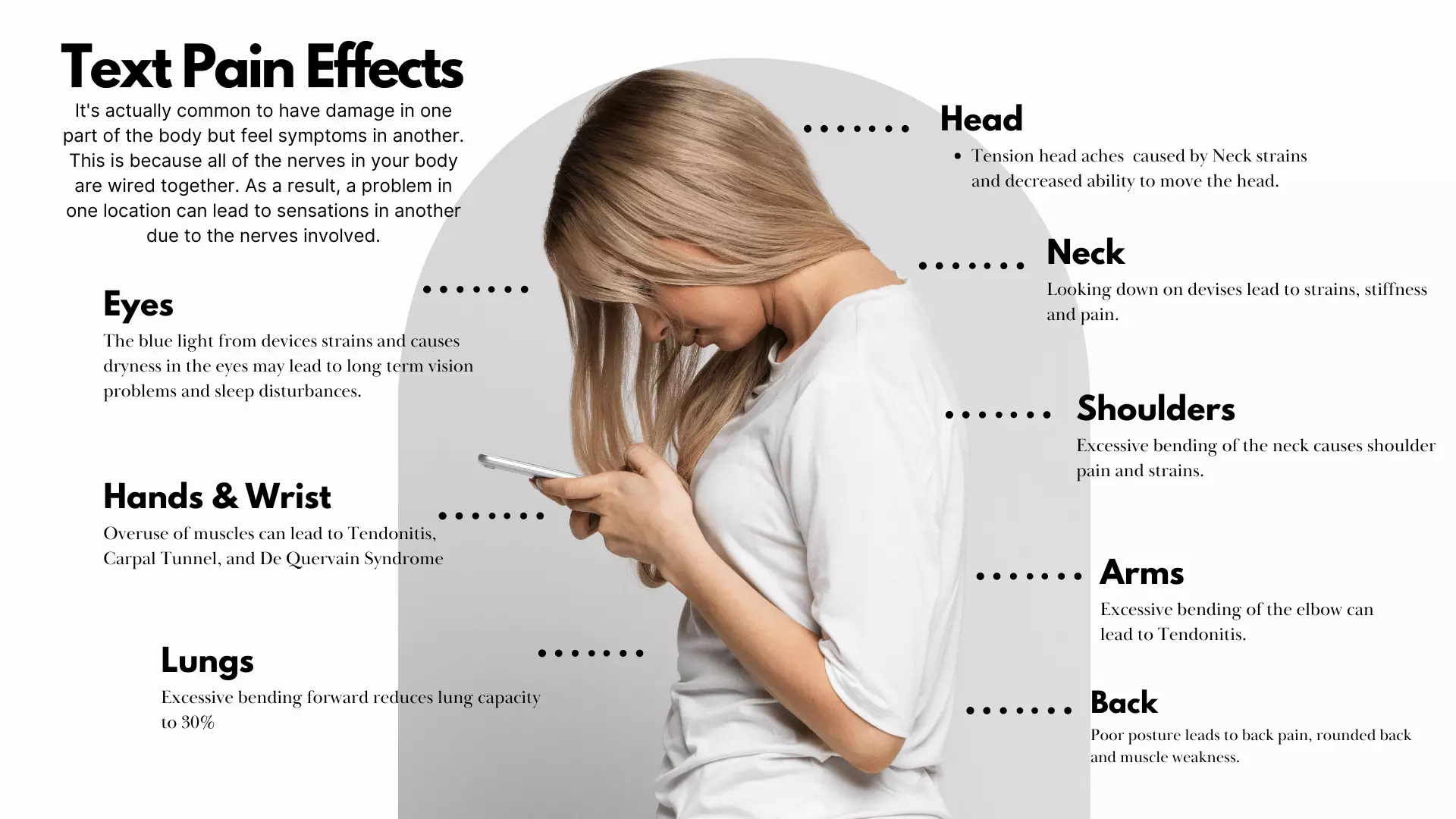
Tips and Tricks to prevent text neck pain
Raise the phone. Move the phone (and other devices) up closer to eye level so the head does not have to be tilted forward.
Take frequent breaks. Take frequent breaks from looking down on your phone.
Watch your posture. With your chin tucked in and shoulders pulled back, this keeps the body aligned in a neutral position.
Arch and stretch. Arch the neck and upper back backward periodically to ease muscle pain.
Stretch and Exercise regularly. A strong, flexible back and neck are more able to handle extra stress.
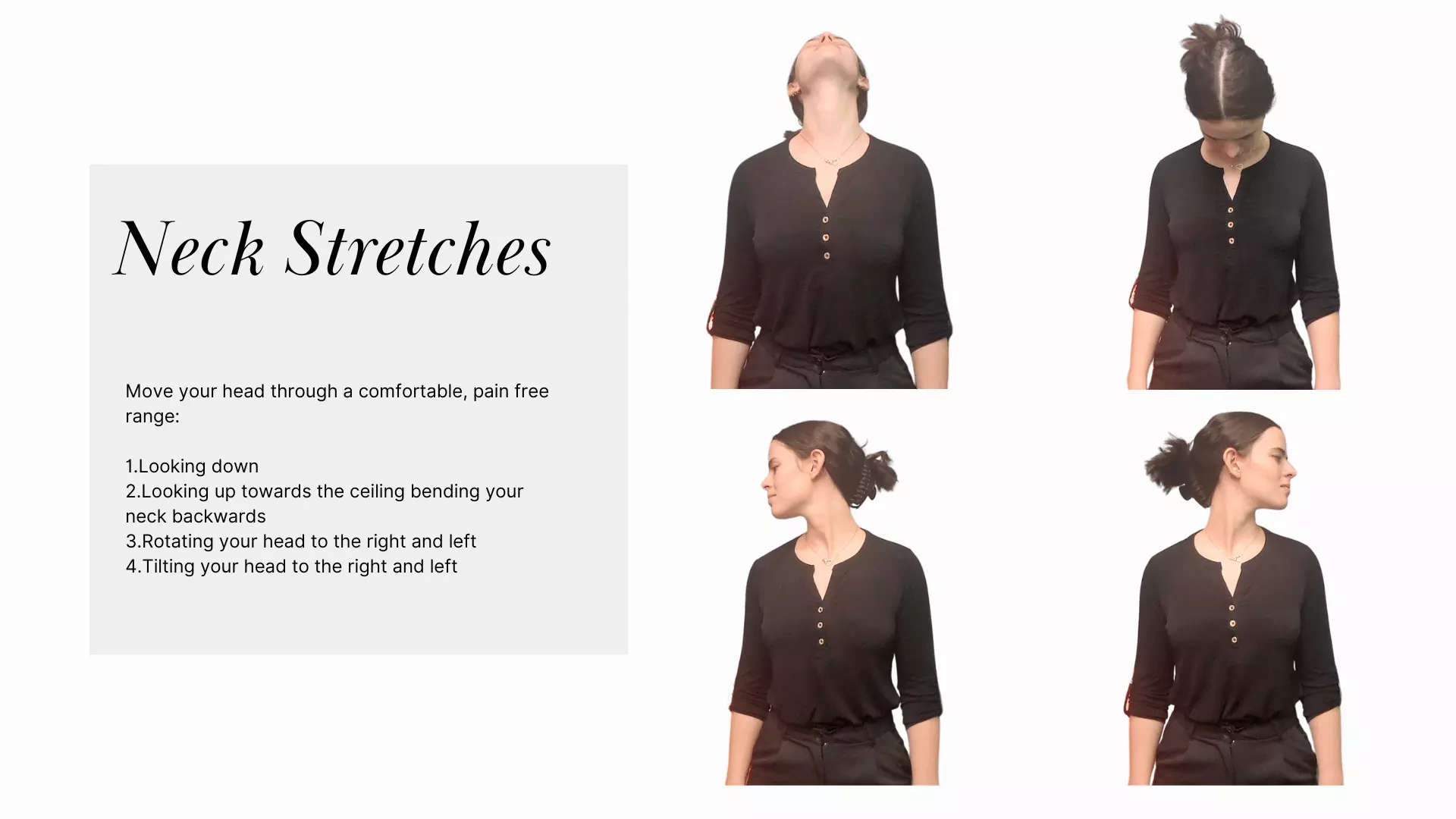
Best Stretches for Neck Pain
You may not be able to completely eliminate looking down at your phone or other devises but we have comprised exercises you can perform that will help relieve some of the pain and tension placed on your neck, back and shoulders.
CHIN TUCK
Chin tucks are typically one of the key exercises recommended for keeping the head aligned above the spine, rather than drifting forward into poor posture. When done regularly and with proper form, chin tucks can help improve the neck’s strength, flexibility, and function.


BENEFITS OF PHYSIOTHERAPY FOR TEXT NECK PAIN
If you’re struggling with neck pain from using your computer or smartphone, it may be time to book an appointment with a physiotherapist to help you develop an individualised treatment plan that aims to improve pain and prevent recurrences.
Physiotherapy treatment for text neck pain comprises of joint mobilization, massage therapy, stretches, and exercises.The physiotherapist would teach you postural techniques to reduce the pain and strains and tightness of muscles and help your body to move freely.

‘Tis the season when the temperature starts to drop causing muscles, tendons and ligaments that support the spine to contract and become stiff. For those with bone and joint related issues, winter weather causes an increase in pain, stiffness, muscle fatigue and inflammation that are harder to control if not treated.
Most common causes of winter back pain?
Decreased activity. Cold weather often mean less exercise and movement that lead to tight muscles, muscle weakness and poor posture.
Winter-related injuries. Such as slip and falls and strenuous tasks as snow shoveling, holiday preparations and winter sports injuries.
Shivering- the body’s natural response to cold that cause muscles to tense up in the cold causing muscle tension in the back leading to pain.
Beat Winter Back Pain with these exercises:
Bird Dog
Click link for the Video Bird Dog Exercise
Side Plank Click
link for the Video Side Plank Exercise
McGill Curl up
link for the Video McGill Curl Up Exercise
If you find that your winter back pain does not go away, various modalities such as hot and cold therapy, warm Epson salt baths, massage therapy and physiotherapy can help relieve your pain.
A physiotherapist plays a significant role in the management of lower back pain, designing a personalised exercise program to improve flexibility, strengthening, improve range of motion and strengthening the core: to maintain your body’s stability and prevent injuries.
If these tip do not help, contact us for a free consultation to determine what treatment would be best beneficial for you.

P-DTR or Proprioceptive Deep Tendon Reflex is a system that identifies and treats dysfunctional muscles, sensory nerve pathways, and receptors. P-DTR was developed by Dr. J. Pollmer, an orthopedic surgeon. P-DTR is based on the latest neuroscience achievements.
P-DTR Physiotherapy treats those with chronic and stubborn recurring pain that have not responded to traditional treatments.
Before explaining further what P-DTR is, we first must understand how pain works. Pain is an important defence mechanism; it warns the body about potential or actual injuries or diseases so that protective actions can be taken.
When you touch a hot stove, receptors called noxious signals send impulses to the spinal cord, which relate the information to the brain. The brain interprets the information as pain, localizes it, and sends back instructions through their receptors for the body to react. These receptors can become sensitized over stimulated or subject to some trauma causing dysfunctions in our nervous system. Dysfunctions cause inaccurate information to be transmitted to the brain, for example, once you injure your knee. Once that issue or injury heals, the receptors may stay sensitive to stimuli like to stretches and pressure because they are trying to protect from future problems. The brain at that point senses any danger it has to create an output leading to pain and weakness.
If you’re suffering from dizziness, vertigo or imbalance as a result of a viral infection, sports-related injury, inner ear disorder, neurological disorder or head injury or and you’re searching for relief, you may benefit from vestibular rehabilitation.
Back pain occurs for many reasons. Many times, the lifestyle choices we make directly impact the alignment of the spinal column, the function of muscles, and the aches and pains we have. Everyday lower back pain can occur for reasons such as the following.
Whiplash is something of a catch-all term for a range of injuries involving the neck, which happens to include neck strain. For the most part, whiplash shows up in sufferers as neck pain, reduced range of motion, and tightness of the muscles.
More...
Four Questions to Ask Your Physiotherapist Before You Decide to Have a Knee Replacement
Written by Super UserHaving a knee replacement surgery is a huge decision. The potential relief you will experience afterward is a powerful incentive, but there are always risks and costs associated with surgery. The best way to make a decision is first to be as informed as possible on the subject. Here are four questions you should ask your physiotherapist before you make any decisions.
How Physiotherapists Can Prevent an Injury Before it Occurs
Written by Super UserAn ounce of prevention is worth a pound of cure! We’ve heard this with respect to illness, but did you know it also applies to physical injury? A physiotherapist in Mississauga can help you prevent injury before it occurs!

